On this page
Genomics is not appropriate for everyone, but if you are interested in how genomics could be used in your care or the care of you child/children, please ask your clinical team about genomics at Alder Hey.
If you decide not to have a genetic test, you will still receive care and support from healthcare professionals
What is genomics?
All living things, from bacteria, to plants, animals and humans, have a genome; ours is made up of DNA. Every person’s genome is around 99.9% the same as everyone else’s, but that 0.1% difference equals around 3 million variations in the DNA.

Humans share around 96% of their DNA with chimpanzees, 90% with mice and 60% with bananas.

DNA is made of nucleic acids. There are 2 single strands of DNA that are twisted into a double helix shape.
The double helix is folded in to chromosomes.
Humans have 23 pairs of chromosomes, the chromosome that makes us male or female is the only chromosome that is not an identical pair.
Some sections of the DNA are called genes which are the ‘coding’ regions, some sections of the DNA are ‘non coding’. Humans have around 20,000 ‘coding’ genes, which create mRNA that creates proteins that are essential for building and repairing all the cells in our bodies.
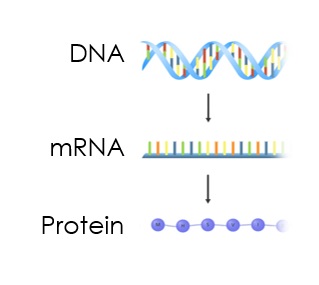
Each chromosome has a copy of each gene; so each person has two copies of each gene, one copy is inherited from the mother and the other from the father.
Some genes determine physical characteristics, such as eye colour, others can influence the chance of developing a health condition, such as cystic fibrosis.
Genetics is the study of genes and their roles in inheritance; the way that certain traits or conditions are passed down in the genes from one generation to the next, like how you can pass blue eyes onto your children.
Genomics is the study of a whole genome; the coding and non coding areas. It looks at how genes are activated to produce proteins, how genes interact with each other and how this information is applied to make organisms growth, develop and function in the right way.
What difference does Genomics make to patient care?
Variation in a persons DNA can be beneficial, harmful, or neutral. Genomic testing allows us to identify any variation.
Genomic tests may be carried out at different times in a person’s life for the following reasons;
- your doctor thinks you might have a health condition caused by a change to 1 or more of your genes
- someone in your family has a health condition that’s caused by changes to genes
- some of your close relatives have had a particular type of cancer that could be inherited
- you or your partner have a health condition that could be passed on to your children
A genomic test can;
- help to diagnose a rare health condition in a child, by comparing DNA in people with and without a condition to find variation that is causing the condition
- help you understand which infectious disease is causing someone to be poorly
- help you understand whether an inherited health condition may affect you, your child or another family member, and help you decide whether to have children.
For example when both parents carry a variant, 1 in 4 children will be affected by the condition - show if you are at higher risk of getting certain health conditions in the future, including some types of cancer
- guide doctors in deciding what specific medicine or treatment to give you. For example a lot of cancers now have targeted therapy that is chosen based on the results of a genomic test
- And where we previously gave all people with a condition the same drugs which didn’t always work and made some people more poorly. We now know that people respond differently and we can personalise the drug amount to different people using the results of a genomic test
- guide doctors on whether you’re able to join a clinical trial
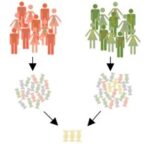
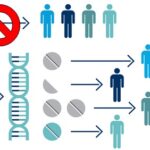
Image descriptions (left to right)
Image 1 – Comparing the DNA of 2 groups of people, one with and one without a health condition to identify the DNA causing the health condition
Image 2 – Previously all people received the same dose of a medicine, now people can receive a normal/lower/higher dose of medicine, or an alternative medicine depending on their DNA
Image 3 – A number of cancers can now be treated with targeted therapy
Patient information
Genomic testing is often done by blood tests. For information on blood tests, please click here.
Below are 3 short videos explaining what will happen when you have a genomic test, and explaining what a microarray test and a panel test are in more detail.
Further information
Why is genomics important to healthcare?
Genomics is revolutionising the way we think about healthcare. It is providing a far more detailed understanding of what causes illness and infectious disease and is helping us develop new treatments that would have been unthinkable even a decade ago.
Over the next ten years the UK Government has the ambition to create the most advanced genomic healthcare system in the world, underpinned by the latest scientific advances, to deliver better health outcomes at lower cost. This vision is set out in the 2020 Government Strategy: Genome UK – the Future of Healthcare. The vision is to support earlier detection and faster diagnoses, use genomics to target interventions to specific groups of patients (personalised medicine), support patients in understanding what genomics means for their health, and bring the full strength of NHS capabilities in this field together against new global pandemics and threats to public health. It will also support fundamental and translational research and ensuring a seamless interface between research and healthcare delivery, making the UK the leading global hub for life sciences. In the 2022 Strategy; Accelerating Genomic Medicine in the NHS the UK government aims to have genomics embedded within the NHS over the next 5 years.
Patients benefit enormously from research and innovation, with breakthroughs enabling prevention of ill-health, earlier diagnosis, more effective treatments, better outcomes and faster recovery. The aims for linking and correlating genomics, clinical data and data from patients to provide routes to new treatments, diagnostic patterns and information to help patients make informed decisions about their care. Genomic testing will support ‘research-active’ hospitals as they have lower mortality rates, with benefits not limited to those patients who participate in research.
Genomics is linked to a number of national strategic documents such as;
- The NHS Long Term Plan from 2019
- The Rare Diseases Action Plan for England from 2022
- The Life Science Vision published in 2021
- Genomics Beyond Health from 2022
What is the NHS Genomic Medicine Service?
To enable the NHS to harness the power of genomic medicine and science to improve the health of our population as part of our commitments in the NHS Long Term Plan; NHS England has commissioned a genomic medicine service to provide equitable access to genomic testing across the country.